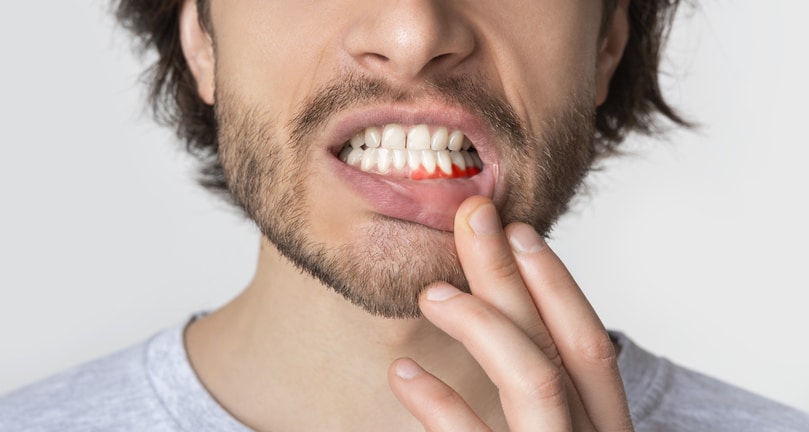
What Is Gingivitis?
Gingivitis is the first stage of periodontal disease. Plaque and its toxic by-products irritate the gums, making them tender, inflamed, and likely to bleed.
What Causes Gingivitis?
Gingivitis is an inflammatory condition that develops in the gums. It is a precursor to advanced gum disease, which can cause the gums to pull away from the teeth and the periodontal ligament to deteriorate. Inflammation in the gums is a direct result of plaque, and plaque formation is the direct result of poor oral hygiene.
When we do not brush and floss well and we do not see the dentist regularly, we set the stage for progressive degradation of the gums:
- Plaque forms on teeth within 24 hours. This is why we are advised to brush morning and night and to floss before bed. Plaque is invisible and odorless. It is a biofilm made primarily of bacteria along with food particles and saliva. The bacteria in plaque feed on the sugar and starches in food particles and create an acidic byproduct that lingers in the mouth.
- Plaque hardens into tartar. When plaque is not adequately removed, it hardens into calculus we know as tartar. Tartar cannot be removed by brushing and flossing. The only way to remove tartar is by scraping it away, which a dentist or dental hygienist does with a special instrument. Because tartar is hardened, it acts as a protective barrier for hidden bacteria.
- Inflammation develops in the gingiva. The gingiva is the upper layer of gum tissue. Inflammation and irritation occur here as a result of prolonged exposure to acidic byproduct produced by bacteria. Inflammation may resolve with increased oral hygiene if addressed early. Otherwise, professional cleaning is necessary to prevent inflammation from progressing to infection.
What Are The Symptoms Of Gingivitis?

- Swelling or puffiness in the gums
- Change in color from light pink to dark or dusky red
- Bleeding when brushing or flossing
- Bad breath
- Tenderness in the gums
- Gums pull away from teeth (gum recession)
Is Gingivitis Contagious?
Studies show that the bacteria that cause inflammation and infection in the gums can live in the saliva. This can make gingivitis contagious between any two people who may share eating utensils, toothbrushes, or other items. Getting prompt treatment for gingivitis could protect everyone in the family.
How Is Gingivitis Diagnosed?
Gingivitis can be diagnosed during a routine dental exam. In this comprehensive evaluation of the teeth and gums, Dr. Holbrook reviews your dental history and looks at all of your teeth and all margins where teeth meet the gums. Where pockets are identified, depth is measured using a small instrument. The depth of periodontal pockets indicates the degree of inflammation and recession that has occurred. Healthy pockets may measure between 1 and 3 millimeters. Deeper pockets suggest that inflammation or infection has developed. Dental x-rays can also help us identify the presence of gingivitis and gum disease.
How Is Gingivitis Treated?
The prompt treatment of gingivitis is vital to successfully reversing symptoms and halting the progression to gum disease and more serious complications. Treatment for gingivitis often involves what is referred to as deep dental cleaning. During a routine dental cleaning, the hygienist uses a rotating instrument to polish teeth and floss to clean in between teeth. A deep cleaning involves techniques referred to as scaling and root planing.
Scaling is the process of removing tartar from tooth surfaces both above and below the gum line. After all tartar and plaque are removed, root planing may be performed to smooth root surfaces that have been made rough by bacterial acid. After this procedure is done, it is imperative to implement good daily hygiene and ongoing professional care to prevent the further decline of oral health.
Is Treatment For Gingivitis Painful?
Gum treatments are performed with a local anesthetic that numbs the treatment area. This is just the same as when you get a dental filing, crown, or root canal. The anesthetic interrupts nerve responses for the duration of treatment and a short period thereafter. Once the numbing medication wears off, mild to moderate tenderness or soreness may occur. This can be managed with over-the-counter or prescription medication.
What Our Patients Have to Say
"My family has been going to Dr. H. for a number of years. Everyone there is professional and friendly, I actually don’t mind going to the dentist. Our family has had various dental needs and they have always been met with positive outcomes. Highly recommend!"
What Is Recovery Like After a Gum Inflammation Treatment?
Patients may need to modify dietary habits for a short time after receiving treatment for gum inflammation or gum disease. We discuss post-treatment recommendations at the time of care based on the procedure that is performed. In most cases, recovery consists of eating softer foods for a few days, taking recommended medications to manage comfort, and carefully brushing and flossing to continue decreasing the adverse effects of oral bacteria.
How Can I Prevent Gingivitis?
It is not difficult to prevent gingivitis. Experts recommend:
- Good daily oral hygiene. People who brush their teeth twice a day for a full two minutes and who floss once a day are less likely to develop gingivitis and gum disease. It is also helpful to rinse the mouth after meals and snacks. Some people also floss first and then brush to remove the fullest extent of debris from the mouth.

- See the dentist. Professional dental exams and cleanings are complementary to daily brushing and flossing. These visits should take place every six months. Based on the findings of a dental checkup, Dr. Holbrook or our hygienist can recommend brushing and flossing tactics to decrease existing inflammation or reduce apparent risks.
- Healthy lifestyle habits also promote optimal oral health. Suggested practices include eating in a way that manages blood sugar and minimizes oral acidity.
- Avoid smoking and tobacco use. These habits have been names as direct influencing factors in the development of gingivitis and a major risk factor in gum disease and periodontitis.
Schedule a Consultation with Dr. Holbrook Today
If you want to learn more about the diagnosis and treatment of gingivitis or would like to schedule a routine checkup and cleaning, call 505-881-1159 to schedule a consultation. Steven E. Holbrook, D.M.D is proud to serve Albuquerque, NM and the surrounding areas.






